The Treatment Ladder
Dermatitis treatment escalates based on severity. Most people start at the bottom. Not everyone needs to climb higher. Here is what works at each level and why.
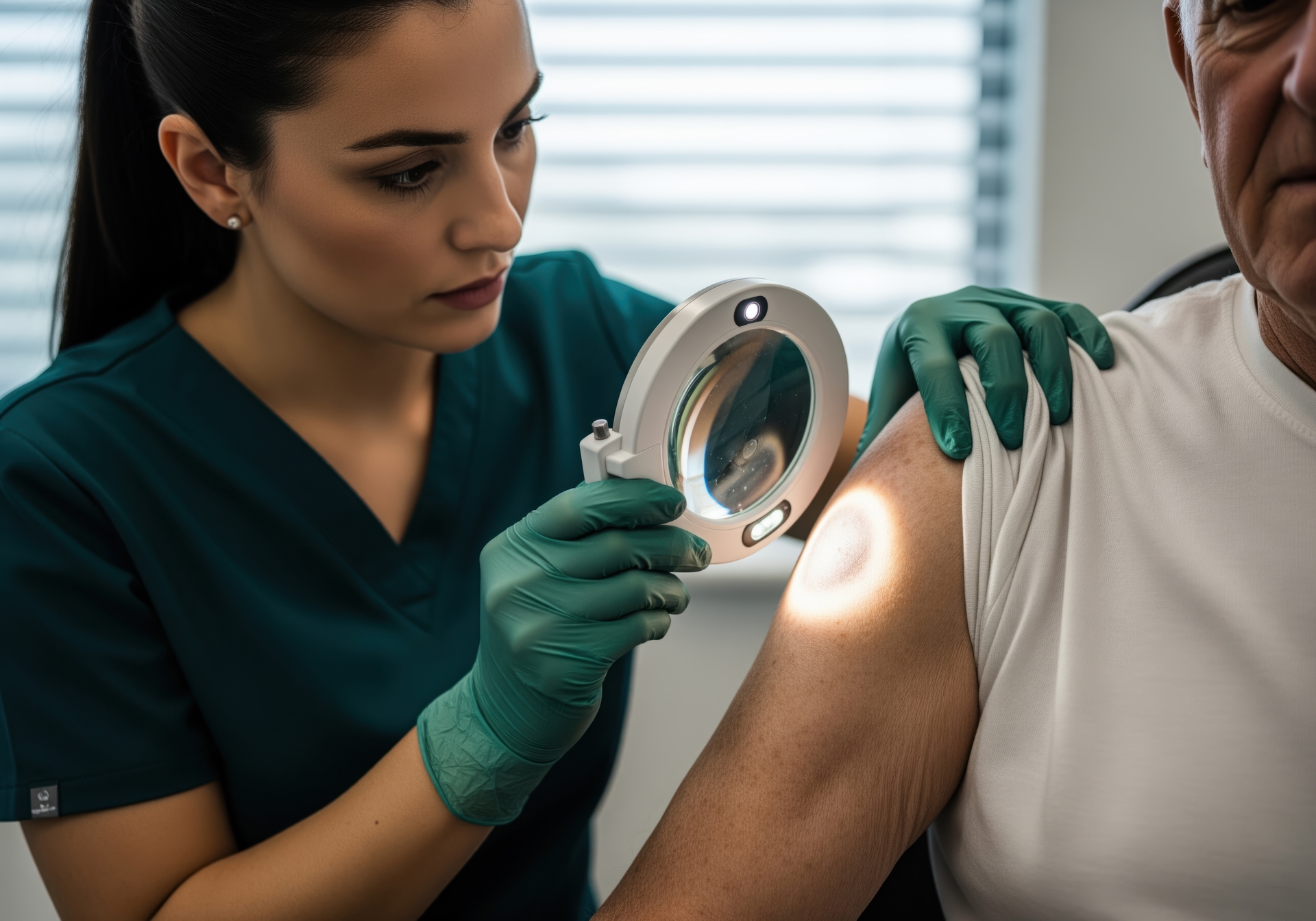
Dermatitis treatment escalates based on severity. Most people start at the bottom. Not everyone needs to climb higher. Here is what works at each level and why.


Ceramide-based creams (CeraVe, Vanicream), petrolatum (Vaseline, Aquaphor), and colloidal oatmeal (Aveeno) form the foundation of every eczema treatment plan. Apply within 3 minutes of bathing to lock in moisture. This isn’t optional supplemental care. Moisturizer is medicine for eczema.
The key distinction is between occlusives (like petrolatum, which seals moisture in), humectants (like glycerin and hyaluronic acid, which draw water to the skin), and emollients (like ceramides, which fill gaps in the skin barrier). The most effective moisturizers combine all three.
Topical corticosteroids remain the workhorse treatment for eczema flares, ranging from mild (hydrocortisone 1%) to superpotent (clobetasol propionate 0.05%). The key is matching potency to body area: low-potency for the face and skin folds, medium for the body, high-potency for thick-skinned areas like palms and soles.
For areas where long-term steroid use is not ideal (face, eyelids, groin), calcineurin inhibitors offer a non-steroidal alternative. Tacrolimus (Protopic) 0.03% and 0.1% and pimecrolimus (Elidel) 1% work by blocking T-cell activation without the thinning risk of steroids.
Steroid phobia is one of the biggest barriers to effective eczema treatment. When used correctly, under medical guidance, with appropriate potency for each body area and with scheduled breaks, topical steroids have an excellent safety profile.
For moderate eczema that doesn’t respond to topicals alone, narrowband UVB (NB-UVB) phototherapy can calm inflammation across large body areas. The treatment works by suppressing the overactive immune cells in the skin and has been a dermatology staple for decades.
Typically administered 2 to 3 times per week in a dermatologist’s office, each session lasts only seconds to minutes. Most patients see improvement within 2 to 3 months. Home phototherapy units are available for patients who cannot make frequent office visits, though they require careful dosing under physician supervision.
Phototherapy is particularly useful as a bridge treatment before stepping up to systemic therapy, or as maintenance for patients who want to minimize medication use.
For moderate to severe eczema that has not responded adequately to topical treatments and/or phototherapy, systemic therapies target the immune pathways driving the disease from the inside out. This category has been revolutionized in recent years.
These treatments have dramatically changed outcomes for patients with severe eczema who previously had limited options beyond cyclosporine and methotrexate (which remain available but carry more significant long-term risks). Check RxSaver.ai for savings programs on biologics and JAK inhibitors, as these medications carry high list prices.
The single biggest mistake I see is steroid phobia. Patients suffer for months because someone online told them topical steroids are dangerous. Used correctly, they’re safe and effective. The real danger is undertreating eczema and letting the itch-scratch cycle destroy your skin.

Have a question about treatment options? Ask our AI assistant.