Atopic Dermatitis
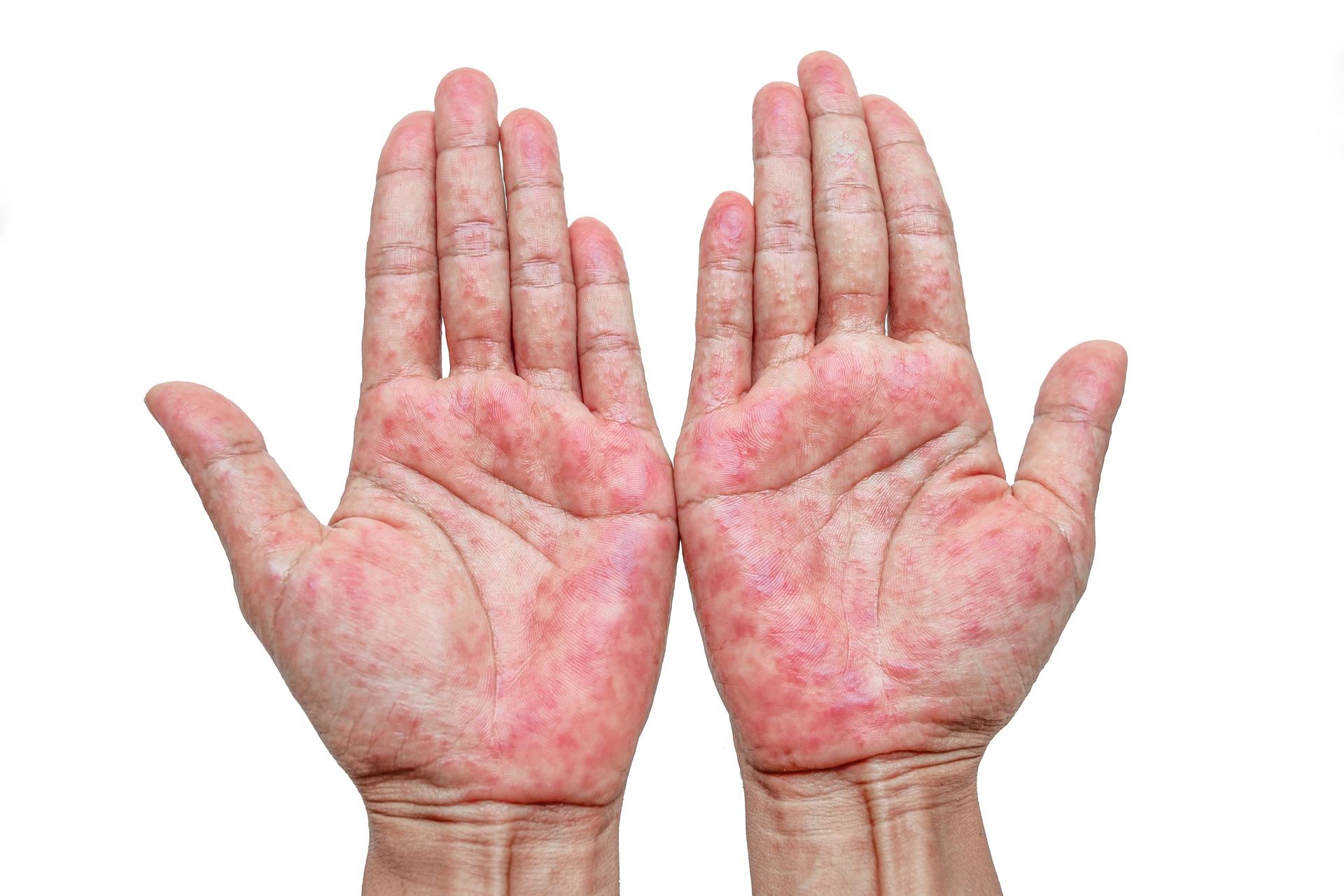
Atopic dermatitis is the most common form of eczema, affecting an estimated 16.5 million U.S. adults and roughly 9.6 million children under 18. It is a chronic, relapsing condition driven by a combination of genetic predisposition, immune dysregulation, and environmental triggers.
The hallmark of atopic dermatitis is a defective skin barrier. In many patients, mutations in the filaggrin gene (FLG) reduce the skin’s ability to retain moisture and keep irritants out. This allows allergens, bacteria, and environmental pollutants to penetrate the outer skin layer, triggering an overactive immune response that produces the characteristic inflammation, redness, and intense itching.
Atopic dermatitis usually begins in infancy or early childhood, often alongside asthma and allergic rhinitis (the “atopic triad”). While many children improve by adolescence, the condition persists into adulthood for a significant portion. In adults, it commonly affects the hands, inner elbows, behind the knees, and the face and neck. Treatment ranges from daily moisturizing and trigger avoidance to prescription topicals, phototherapy, and biologics for severe cases.
Contact Dermatitis
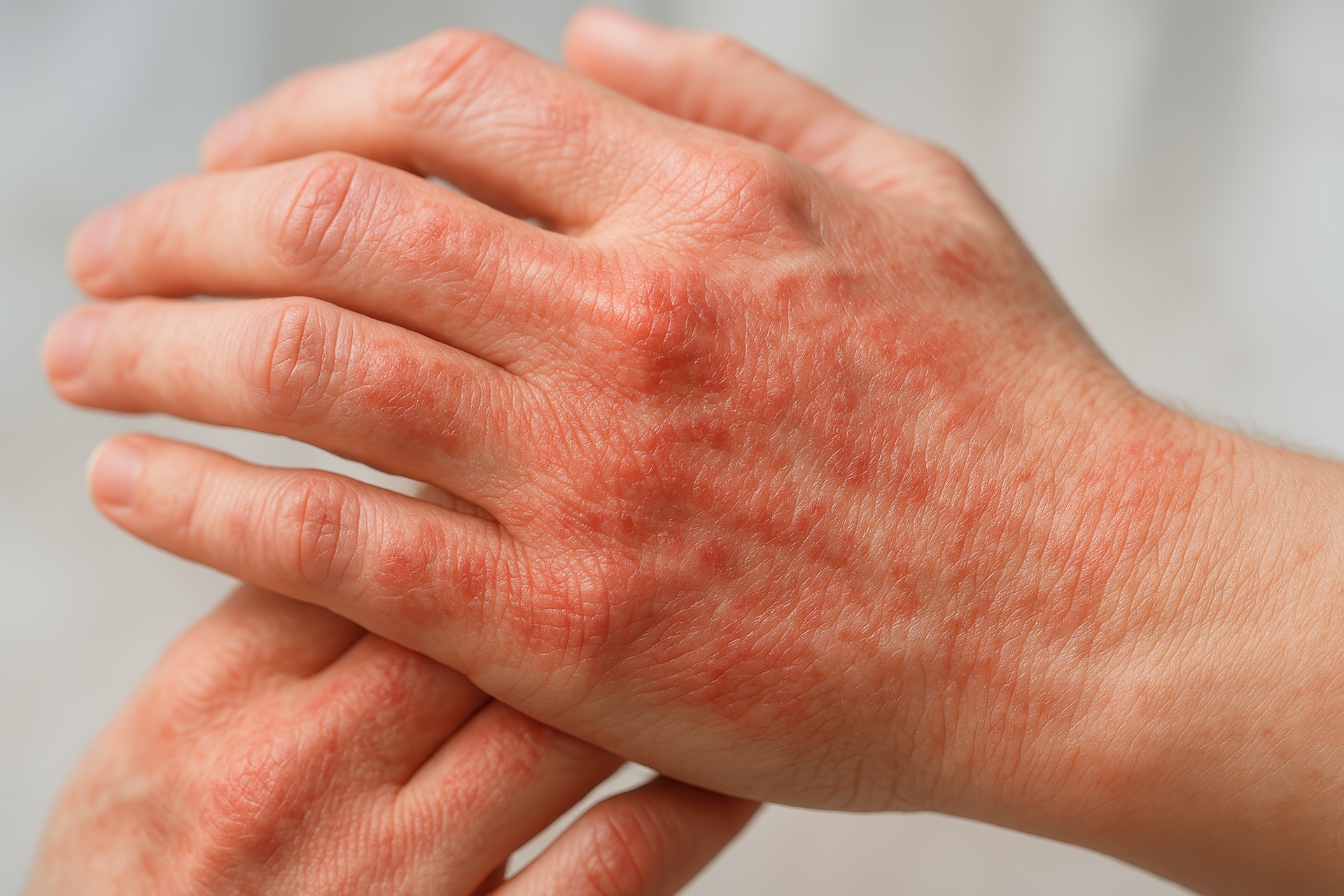
Contact dermatitis occurs when your skin reacts to a substance it has touched. There are two main subtypes: allergic contact dermatitis (an immune-mediated delayed hypersensitivity reaction) and irritant contact dermatitis (direct chemical damage to the skin without immune involvement).
Allergic contact dermatitis is caused by sensitization to specific allergens. Common culprits include nickel (jewelry, belt buckles), fragrance compounds, preservatives like formaldehyde and methylisothiazolinone, latex, and urushiol (poison ivy/oak). Once sensitized, even trace exposure can trigger a reaction. Diagnosis requires patch testing, where small amounts of common allergens are applied to the back under adhesive for 48 hours and read at 48 and 96 hours.
Irritant contact dermatitis, the more common form, results from repeated exposure to substances that damage the skin barrier without triggering an immune response. Frequent handwashing, detergents, solvents, and acids are typical causes. Healthcare workers, hairdressers, food handlers, and mechanics are at elevated risk. Treatment centers on identifying and avoiding the causative substance, repairing the skin barrier, and using topical corticosteroids for active inflammation.
Seborrheic Dermatitis

Seborrheic dermatitis produces flaky, scaly, sometimes greasy patches on areas of the skin with high sebaceous (oil) gland density: the scalp, face (especially around the nose and eyebrows), ears, and chest. In infants, it appears as “cradle cap.” In adults, most people simply know it as persistent dandruff.
The condition is closely associated with Malassezia, a genus of yeast that naturally colonizes human skin. In susceptible individuals, the yeast triggers an inflammatory response in oil-rich skin areas. Seborrheic dermatitis tends to flare with stress, cold and dry weather, illness, and fatigue. It is more common and often more severe in people with HIV/AIDS, Parkinson’s disease, and other neurological conditions.
Treatment typically involves antifungal agents (ketoconazole, selenium sulfide, zinc pyrithione) in shampoo or cream form, along with low-potency topical corticosteroids for flares. Calcineurin inhibitors like tacrolimus or pimecrolimus are useful for facial involvement where long-term steroid use is not ideal. Seborrheic dermatitis is manageable but usually recurrent; most patients need ongoing maintenance therapy.
Nummular Dermatitis
Nummular dermatitis (also called discoid eczema) produces distinctive coin-shaped patches of inflamed, itchy skin. The lesions are well-defined, round to oval, and can range from a few millimeters to several centimeters in diameter. They often appear on the arms, legs, and torso.
This form of dermatitis is frequently mistaken for ringworm (tinea corporis) due to the circular shape, but unlike ringworm, nummular dermatitis is not caused by a fungal infection. Triggers include very dry skin, insect bites, skin trauma (cuts, burns, abrasions), and contact allergens. It is more common in winter months when indoor heating dries the air.
Nummular dermatitis tends to be more stubborn than other eczema types. Treatment involves aggressive moisturizing, medium- to high-potency topical corticosteroids, and addressing underlying skin dryness. In resistant cases, phototherapy or short courses of systemic immunosuppressants may be needed. Patients should be counseled that lesions may take weeks to fully resolve and that brown post-inflammatory marks may persist for months after the inflammation has cleared.
Dyshidrotic Eczema
Dyshidrotic eczema (pompholyx) produces small, intensely itchy, fluid-filled blisters on the palms, sides of the fingers, and soles of the feet. The blisters are typically deep-seated, giving the skin a “tapioca pudding” appearance. They may coalesce into larger bullae in severe cases.
Despite the name, dyshidrotic eczema is not caused by sweat gland dysfunction (as was once believed). It is associated with atopic dermatitis, contact allergens (especially nickel and cobalt), stress, seasonal allergies, and excessive hand moisture or sweating. It is one of the most underdiagnosed forms of eczema, and many patients live with it for years before receiving proper treatment.
Acute flares are treated with high-potency topical corticosteroids and cold compresses. For chronic or recurrent cases, calcineurin inhibitors, phototherapy (PUVA soaks for hands), or short courses of oral steroids may be prescribed. Identifying and avoiding contact allergens through patch testing is important for patients with recurrent episodes. Keeping hands dry and using barrier creams for wet work can help prevent flares.
Stasis Dermatitis
Stasis dermatitis (gravitational eczema, venous eczema) develops on the lower legs in the setting of chronic venous insufficiency. When leg veins fail to efficiently return blood to the heart, pressure builds in the lower extremities, causing fluid to leak into surrounding tissue. This triggers inflammation, itching, and skin changes.
Early signs include ankle swelling, a dull aching or heaviness in the legs (especially after prolonged standing), and mild redness or scaling around the ankles. As the condition progresses, the skin may become darkened (hemosiderin staining from red blood cell breakdown), thickened, and fibrotic. In advanced cases, the skin can break down into venous leg ulcers, which are notoriously difficult to heal.
Treatment of stasis dermatitis requires addressing both the skin inflammation and the underlying venous insufficiency. Compression therapy (graduated compression stockings or wraps) is the cornerstone of management. Topical corticosteroids treat active inflammation. Leg elevation, regular walking, and weight management support venous return. Patients with stasis dermatitis should avoid standing for prolonged periods and be evaluated for correctable venous disease. It is important to differentiate stasis dermatitis from cellulitis, which requires antibiotic treatment.